TREATMENT - MYOMA
WHAT YOU NEED TO KNOW ABOUT MYOMAS
Myomas are benign tumours of the muscle tissue, which are not dangerous in themselves, but they need to be treated because of the mild to severe complications caused by the nodule. The myoma nodules mostly consist of connective tissue and muscle tissue and they can be singular or multiple; in some cases more than one nodule can be present in the same organ. Their size may vary from seedlings to bulky masses which can grown to the size of a watermelon. Myomas rarely occur in striated muscle, they most often appear as uterine fibroids in the smooth muscle of the uterus. Its development and growth is supposedly connected to activity of the ovaries. Myomas develop during childbearing years, often after the age of 25 to 30, and is one of the most frequent gynaecological conditions.
WHERE DO MYOMAS DEVELOP?
Myomas can be submucosal (bulging into the uterine cavity), intramural (within the muscular uterine wall) or subserosal (on the outside of the uterus) depending on which part of the uterus they develop in. Patients with myomas may have a variety of symptoms: pelvic pain that may radiate towards the back and the legs, menstruation disorders, vaginal discharge, pressure, mainly on the intestines and the bladder, which may cause urinary and defecation problems, complicated pregnancy, birth complications, infertility etc.
Factors that make people prone to develop myomas are not yet fully known, but it is probable that female sex hormones play an important role. This theory is supported by the fact that during estrogen treatment and pregnancy myomas tend to grow.
After the menopause, developed myomas may withdraw. However, following the last period it is still imperative to have regular gynaecological examinations. Myomas are most often detected during routine gynaecological examinations or abdominal ultrasound examinations.
Myomas often cause no symptoms. However, depending on their location and the size, it can cause various symptoms, which are in most cases mild, but can cause problems in daily life. Such problems can be vaginal discharge, pain and bleeding. In some cases thus benign nodule can cause severe symptoms. A large myoma may press against the bladder causing recurring urinary tract infections or even incontinence problems.
Smaller myomas that do not cause symptoms are most often detected during routine gynaecological examinations or abdominal ultrasound examinations. (In some cases laparoscopy, a camera examination of the organs inside the abdomen, may also be necessary for a certain diagnosis.) That is the reason why it is worth attending screening examinations regularly, and detected nodules must be checked regularly, because in cases of extremely rapid growth, the myoma may become malignant, although the probability for this is rather low (if you experience pelvic pain of unknown origin or palpable mass or swelling, consult your gynaecologist immediately). If you have bladder or bowel issues, changed or irregular periods, you will also need an immediate checkup.
Depending on the severity of the symbols and the patient’s age, the myoma may be treated with medications or hormones, can be removed surgically or through catheter embolization. The applied surgical procedures can be traditional or radical operations. The surgery can be performed through the vagina or through an incision in the abdomen, and often the entire uterus is removed.
MYOMA EMBOLIZATION
During traditional surgery removing myomas, often the whole uterus is removed. Thanks to the embolization technique available at our institute, the uterus will not be removed, and the treatment causes only minimum stress for the body, as it is performed without anaesthesia and incisions.
The state-of-the-art embolization procedure is performed in an angiography operating theatre; after applying local anaesthesia at the elbow crease, a thin catheter will be introduced into the artery through a single puncture. Uterus is supplied with blood through a singular vein from both the left and right pelvic arteries, which will be dyed applying contrast agent in the first step. This may cause a warm sensation in the pelvic area and may cause a stimulus for urination. It is necessary for us to detect the exact location and blood supply of the myoma. Then the catheter will be introduced into the veins supplying the uterus with blood, first on one and then on the other side, so we can get as close to the veins supplying the myoma with blood as possible. Through the catheter we inject tiny PVA (polyvinyl alcohol) particles or microbeads into the veins on either side. The beads block the veins that supply blood to the myoma which results in the shrinking and necrosis of the myoma tissue.
Embolization usually takes 30-40 minutes. During the procedure we keep you informed about the procedure and we will let you know when to prepare for a warm sensation. During the procedure no risk factors are to be expected, as we only perform a puncture and there is no need for anaesthesia.
Zoltán Harmat MD, expert interventional radiologist has performed nearly 2000 successful myoma embolizations. CLICK HERE to learn more about Zoltán Harmat MD.
WHAT HAPPENS BEFORE THE PROCEDURE?
At the first consultation we will answer all your questions with regard to the embolization, and our expert will provide thorough information about the procedure. We suggest that you think about the questions you wish to ask in advance, and we will be more than happy to provide the answers. The success of the procedure does not depend on your menstruation cycle, but the best time to perform the operation is the first or second week following your menstruation. After the first examination we will make an appointment for the procedure.
During the first consultation an abdominal ultrasound scan will be performed in order to establish whether or not the embolization can be performed and with what success rate. It can be established to what extent the myoma or myomas can be expected to shrink or whether or not the myoma(s) will be fully absorbed as a result of the procedure. If the ultrasound examination fails to deliver unambiguous results about the state of the uterus and the location, viability and vascularity of the myomas, a magnetic resonance imaging scan (MRI) will be necessary. We will of course help to organize the scan.
When we make an appointment, we shall also discuss the preliminary examinations that need to be performed (Complete Blood Count, coagulation, renal function) and we shall establish whether it is necessary to give you antibiotics treatment or a preliminary anaesthesiology consultation.
WHERE DO WE PERFORM THE EMBOLIZATION?
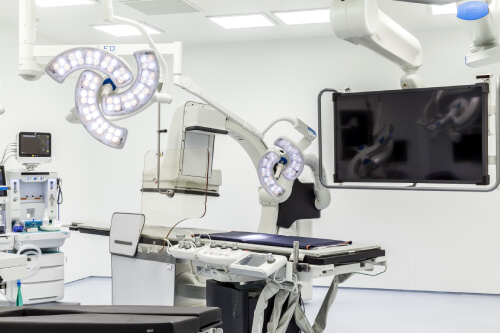
The procedure will be performed in a 50 square metre hybrid operating room (where both imaging and surgeries can be performed). In the Central European private healthcare sector, our facility is the only one that boasts a hybrid operating room.
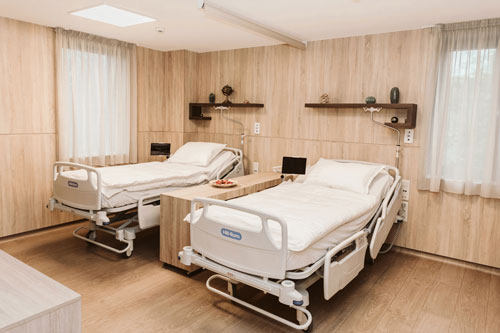
During your stay for the night following the procedure, you will enjoy all the conveniences a five-star hotel room has to offer.
WHAT HAPPENS AFTER THE PROCEDURE?
The procedure must be performed on an empty stomach, therefore we kindly ask you not to have breakfast; you can, however, drink before the procedure. If you take regular medications, feel free to do so in the morning of the embolization. We will inform you of the medicines you should not take during the preliminary consultations.
Upon your arrival at the health centre, you will be escorted to a room, which satisfies all expectations and then we will ask you to read the Declaration of consent. If you agree to sign the document, your blood pressure will be taken, a cannula will be introduced into your left forearm, and you will be shortly escorted into the operating room where the embolization procedure will start.
During the procedure local anaesthesia will be applied at your right elbow crease, which will necessitate a needle puncture. After this you may feel a warm sensation caused by the dye injected in order to perform angiography, but you will not feel any pain. Embolization usually takes 30-40 minutes. During the procedure we keep you informed about the procedure and we will let you know when to prepare for a warm sensation. If you have any unpleasant sensations or have questions during the procedure, we can discuss those.
Once the procedure is over, you will receive analgesic injection and IV therapy; then the catheter will be removed from the right elbow crease, the artery will be compressed for about 15 minutes, then a compressing bandage will be placed on the forearm to fully stop the bleeding at the catheter site. This bandage will stay on the elbow crease for 6 hours.
Following the embolization the partly temporary cessation of the blood supply to the uterus is likely to cause strong spasms in the lower abdomen. Analgesics will certainly decrease the pain, but it is highly probable that you will be experiencing some degree of pain. You can expect to feel the spasm in the first 3-4 hours following the embolization. During this time you can only consume liquids, and can eat solids only later. You will be provided lunch, dinner and the next morning, breakfast at the Health Centre.
You will have to spend the day of the embolization at the Health Centre. The next morning you will participate in a follow-up ultrasound examination, when we check the success of the embolization. During the examination we will inform you about what to do next, the pain you can expect and we can discuss any questions you may have after the procedure. We will hand over all results and documentation to you and at 8 am the next morning you may leave the Health Centre.
CONSULT WITH OUR EXPERTS SO WE CAN HELP YOU!
Choose us and minimize the waiting time for treatment. We can give you an appointment at the earliest convenience.
OUR PHYSICIANS

DR. HARMAT ZOLTÁN
Interventional radiologist, regional radiologist, chief clinical physician
THE CONDITIONS OF THE EMBOLIZATION
A preliminary abdominal ultrasound scan will be necessary in order to establish whether or not the embolization can be performed and with what success rate. It can be established to what extent the myoma or myomas can be expected to shrink or whether or not the myoma(s) will be fully absorbed as a result of the procedure. If the ultrasound examination fails to deliver unambiguous results about the state of the uterus and the location, viability and vascularity of the myomas, a magnetic resonance imaging scan (MRI) will be necessary. We will of course help to organize the scan.
Myomas can be submucosal (bulging into the uterine cavity), intramural (inside the uterine wall) or subserosal (on the outside of the uterus) depending on which part of the uterus they develop in. Patients with myomas may have a variety of symptoms: pelvic pain that may radiate towards the back and the legs, menstruation disorders, vaginal discharge, pressure, mainly on the intestines and the bladder, which may cause urinary and defecation problems, complicated pregnancy, birth complications, infertility etc.
In order to perform the embolization you will need new CBC (Complete Blood Count) results and blood coagulation lab test results, which are the easiest to obtain through your GP. Depending on the size and location of the myoma you may need to take antibiotics.

